Which of the following is an absolute contraindication for placing dental implants?
What is the least common site for development of oral cancer?
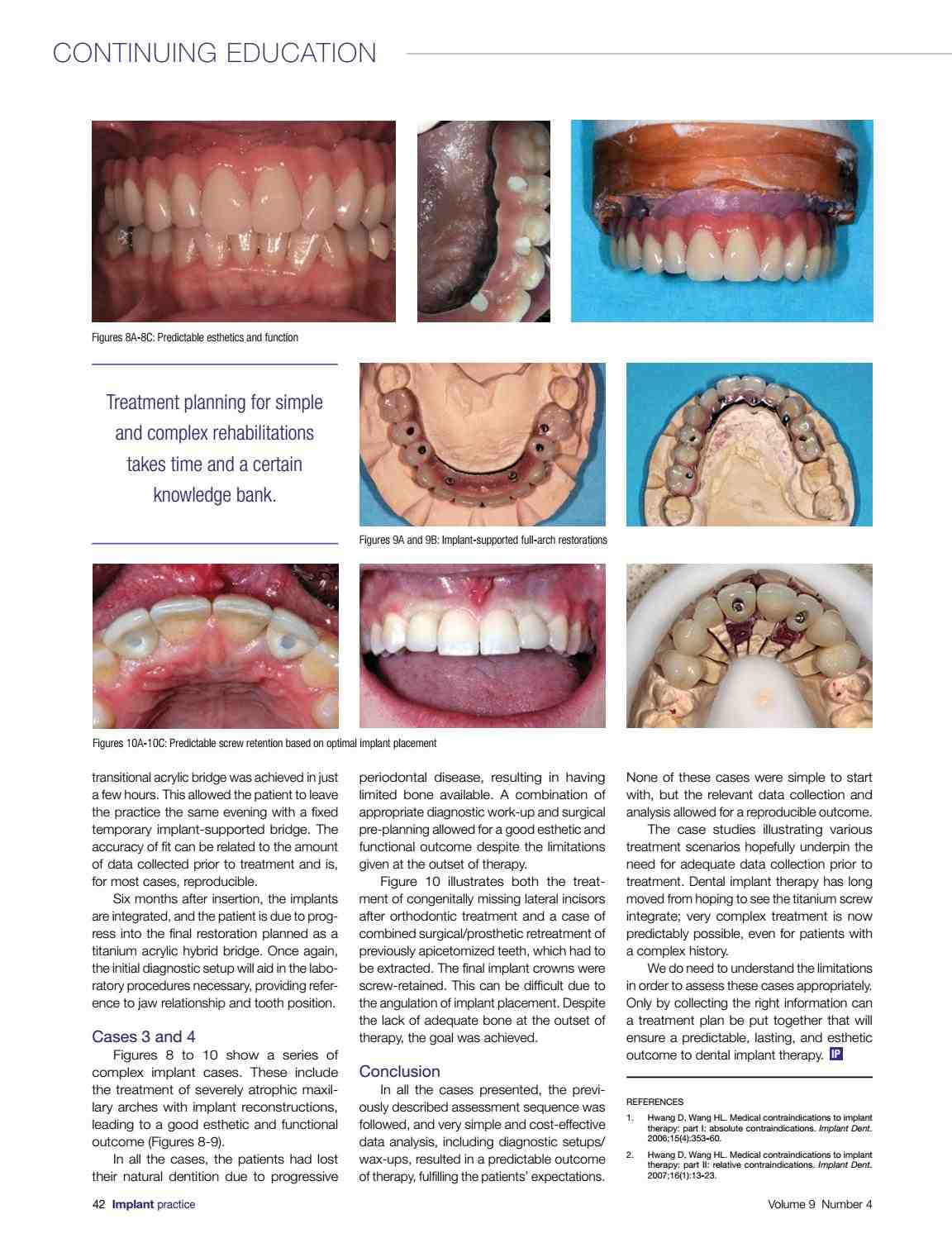
The bottom of the mouth is the second most common intraoral location. Less common sites include gingiva, buccal mucosa, labial mucosa, and hard palate. See the article : Fake Tooth Options. Setting the stage of oral cancer is important to establish proper treatment and prognosis.
Where does mouth cancer usually start?
Mouth cancer usually starts in flat, thin cells (squamous cells) that line your lips and the inside of your mouth. See the article : Could dental implant hit nerve.
How long does it take for mouth cancer to develop?
Fact: Most cases of oral cancer are found in patients over the age of 50 because it often takes many years for this form of the disease to develop. On the same subject : Does blue cross cover dental implants. However, the number of cases associated with HPV and oral cancer is growing over the years and puts younger people at higher risk.
What are the signs of cancer of the tongue?
What are the symptoms of tongue cancer?
- a red or white spot on the tongue that will not go away.
- a sore throat that does not go away.
- a sore spot (ulcer) or a lump on the tongue that does not go away.
- pain on swallowing.
- numbness in the mouth that will not go away
Which of the following dental procedures does not requires antibiotic prophylaxis for individuals at high risk of bacterial endocarditis?

The following dental procedures do not require prophylaxis of endocarditis: Routine injections of anesthetic through uninfected tissue. X-rays of teeth. Installation of removable prosthetic or orthodontic appliances.
What antibiotics treat endocarditis?
Initial empirical therapy in patients with suspected endocarditis should include vancomycin or ampicillin / sulbactam (Unasyn) plus aminoglycoside (plus rifampin in patients with prosthetic valves). Valve replacement should be considered in selected patients with infective endocarditis.
What antibiotic is used for dental prophylaxis?
For oral and dental procedures, the standard prophylactic regimen is one dose of oral amoxicillin (2 g in adults and 50 mg per kg in children), but an additional dose is no longer recommended. Clindamycin and other alternatives are recommended for use in patients who are allergic to penicillin.
Why do I have to take an antibiotic before dental work?
What is antibiotic prophylaxis? Antibiotic prophylaxis (or premedication) is simply taking antibiotics before some dental procedures, such as brushing teeth, extracting teeth, root canals, and deep cleaning between the root of the tooth and the gums to prevent infection.
Which antibiotic is the drug of choice for intraoral infection?

Penicillin is the drug of choice in the treatment of odontogenic infections because it is prone to gram-positive aerobes and intraoral anaerobes, organisms found in alveolar abscess, periodontal abscess, and necrotic pulps. Both aerobic and anaerobic microorganisms are sensitive to penicillin [9].
Which antibiotic is good for tooth infection?
Antibiotics of the penicillin class, such as penicillin and amoxicillin, are most commonly used to treat dental infections. For some types of bacterial infections, the antibiotic metronidazole may be given. It is sometimes prescribed with penicillin to cover a larger number of bacterial species.
What is the alternative to amoxicillin?
For those patients with mild sensitivity to amoxicillin, acceptable alternatives include cefdinir (Omnicef), cefpodoxime (Cefzil), or cefuroxime (Ceftin). These agents, along with amoxicillin clavulanate (Augmentin), are also commonly used as second- or third-line therapy.
What is the best antibiotic for a bacterial infection?
Bacterial infections are treated with antibiotics such as amoxicillin, erythromycin and ciprofloxacin.
When should an avulsed tooth be optimally reimplanted?

Immediate transplantation provides the best possible prognosis, but is not always possible because more serious injuries may be present. Studies have shown that teeth protected in a physiologically ideal medium can be transplanted within 15 minutes to an hour after an accident with a good prognosis.
How long does an avulsed tooth take to heal?
How long does it take to heal a tooth? If the bone around the tooth is not broken, the tooth will be firmly attached to the bone in about three to four weeks. However, if the damage was more significant, it can take six to eight weeks to recover.
What happens when a tooth is avulsed?
Impulsed teeth are teeth that are completely ejected from the groove. Avulsion results in hypoxia and necrosis of the tooth pulp. Reimplantation is the main goal of emergency care, to preserve the periodontal ligament attached to the roots.


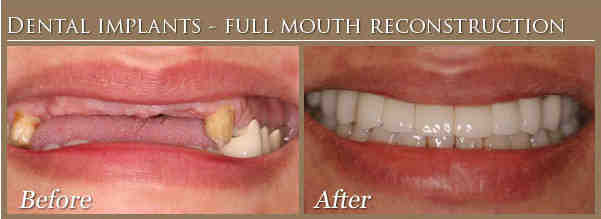
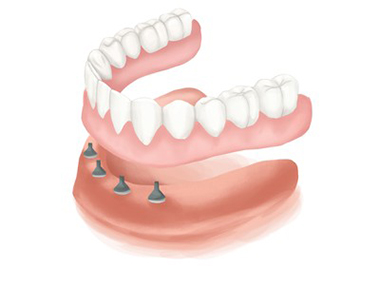


Comments are closed.